Cardio-Pulmonary Perfusionist Salary in the United States
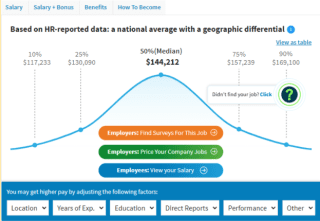
How much does a Cardio-Pulmonary Perfusionist make in the United States? The average Cardio-Pulmonary Perfusionist salary in the United States is $144,212 as of December 27, 2021, but the range typically falls between $130,090 and $157,239. Salary ranges can vary widely depending on many important factors, including education, certifications, additional skills, the number of years you have spent in your profession. With more online, real-time compensation data than any other website, Salary.com helps you determine your exact pay target.
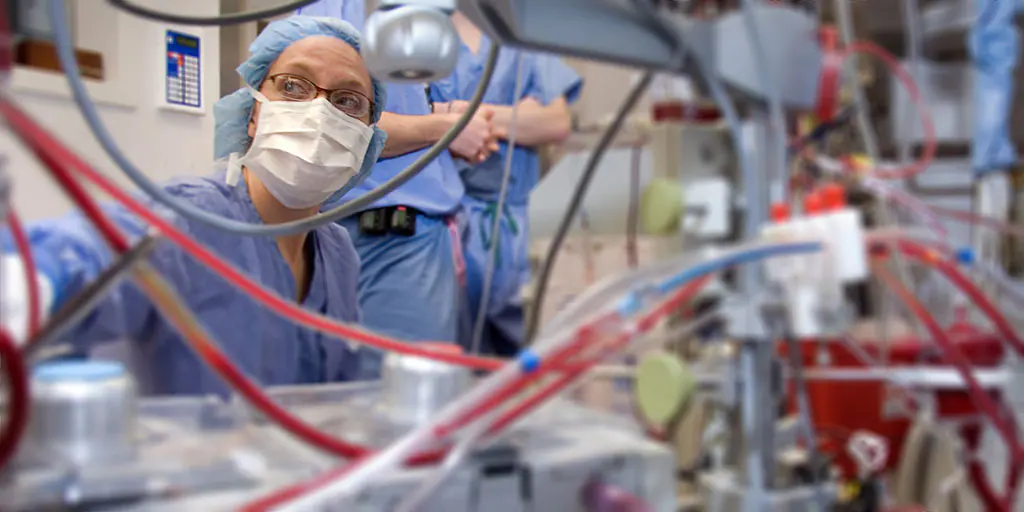
JOB DESCRIPTION FOR CARDIO-PULMONARY PERFUSIONIST
Cardio-Pulmonary Perfusionist sets up and operates heart/lung machines that support organ function during cardiac surgery or other procedures where circulatory or respiratory function is disrupted. Operates equipment to produce bypass, coronary perfusion, recirculation or partial bypass, or to alter blood temperature, balance, or content. Being a Cardio-Pulmonary Perfusionist requires an advanced degree. Requires a Certified Clinical Perfusionist (CCP) credential. Additionally, Cardio-Pulmonary Perfusionists typically report to a manager or head of a unit/department. Cardio-Pulmonary Perfusionist’s years of experience requirement may be unspecified. Certification and/or licensing in the position’s specialty is the main requirement.